Are you confident diagnosing and managing eczema in patients with skin of colour (SOC)?
.jpg)
Gain the skills to diagnose and manage patients with musculoskeletal conditions and sports injuries in primary care.
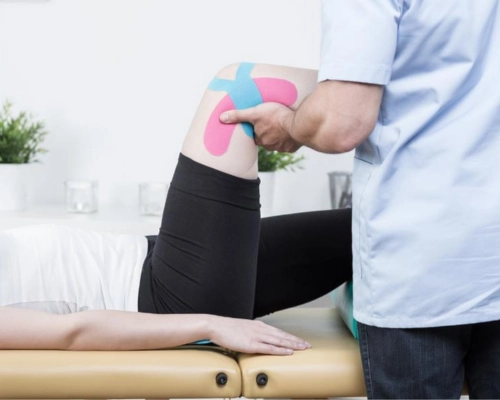
Diagnose musculoskeletal pains and their underlying causes, including joint pain, rheumatoid arthritis, sports injuries, neck injuries, lower limb and gait problems, back pain, and more.
- Perfect for practitioners with no to little prior training in this area.
- This course is for doctors and degree-qualified medical practitioners.
- CPD-accredited and university-assured.
Fulfils 50 hrs for medical professionals in Australia*
100% online
Online + workshop
Workshop only
Fully online: $1695
Online + workshop: from $3190
Workshop only: from $1495
Special rates available
85.5 hrs
Self-paced
2026
20 September in Sydney
*provided an outcome measurement activity with a minimum of 5 hours is completed.

- Meet patient demand, as musculoskeletal conditions account for over 14 per cent of GP encounters and are the third most common reason for presentation.
- Provide your patients with immediate care by addressing common ailments in general practice.
- Assess and minimise risk of cervical spinal cord or nerve root damage.
- Provide long-term support for your patients with ongoing joint and musculoskeletal pains and sporting injuries.
- Judge when to refer on a patient, and learn how to work collaboratively with specialists and physiotherapists.
Get unlimited access to all course content, additional learning materials, ongoing post-course support, and more.
|
Topics covered in the optional skills workshop:
|
This musculoskeletal module focuses on the different types of musculoskeletal pain and its underlying causes. It discusses the pathophysiology of muscular deficiencies commonly seen in general practice in detail, such as muscular overload, muscle pairing imbalance and joint instability. The module then covers the types of treatment and exercise to be applied to these deficiencies. Various images and case studies are presented throughout the module to assist with learning.
This musculoskeletal module focuses on the steps used to initiate a diagnosis in patients with acutely painful joints and briefly introduces the causes and complications of polyarthritis. It outlines the differential diagnosis based on history taking, examinations and investigations. The module explains the epidemiology, aetiology, pathophysiology, natural history and diagnostic criteria of rheumatoid arthritis. The module concludes with the examination, investigations, diagnosis, and management specific to rheumatoid arthritis. Various images and statistics are used throughout the module to assist with learning.
This module focuses on the initial diagnosis and GP management of sport-related neck injuries. It outlines the neck anatomy and common causes of neck injuries in sport. The module then outlines the step-by-step diagnostic process to exclude the possibility of an unstable cervical spine injury that could lead to spinal cord compression and neurological compromise. This involves a combination of history taking, physical findings and, when required, imaging studies. Treatment and management of neck injuries in emergency and uncomplicated situations are discussed. The module concludes with the management of neck injuries in special situations including neck injuries in children, arthritic spine, aging spine and soft tissue injuries with blunt injuries.
This module introduces the definition of musculoskeletal injuries and outlines the role and importance of GP involvement in managing these injuries. The module outlines the different classifications and management of injuries including soft-tissue injuries and closed injuries. It also discusses the principles to improve and optimise the healing of such injuries. The module then focuses on the diagnosis and management of common musculoskeletal injuries including ankle sprains, syndesmosis injuries, MCL injuries, hamstring tears, groin strains and adhesive capsulitis. The module concludes with the diagnosis and symptoms of concussion and ways to manage them.
This musculoskeletal module begins with an introduction to the principles and fundamentals of biomechanical assessments. Terminology and assessment tips of a normal gait are outlined including movement, forces and pressures. It also discusses the terminology and clinical symptoms of antalgic/abnormal gait of the hip, knee, ankle and foot. The module then discusses the biomechanical assessments of the lower limb including non-clinical gait tests, altered/additional gait tests, ankle D/F lunge tests and other quick tests. The management and therapeutic intervention of the lower limbs is outlined. The module concludes with referral options and when and whom to refer patients. Various images are presented throughout the module to assist with learning.
This musculoskeletal module focuses on planning an assessment of patients with chronic joint pain and degenerative joint disease. It begins with an introduction and overview of arthritis and a discussion on the differential diagnoses of degenerative joint and inflammatory joint disease. The module explains the epidemiology, pathogenesis, clinical features and diagnosis of osteoarthritis (OA). Overarching principles of OA management are discussed including OA management of the hip, knee and hand. The module concludes with the management of cervical and lumbar spondylosis.
This musculoskeletal module focuses on the initial diagnoses and management of low back pain including GP assessment for cauda equina or spinal nerve root damage. It outlines the epidemiology, definitions, anatomy and physiology of low back pain including red flags that require urgent intervention. Patients that need investigations through relevant lab tests are discussed. Different imaging modalities including X rays, CT scans, MRI, bone scans and Nerve Conduction Studies are outlined depending on the symptoms. The module concludes with the management of non-specific low back pain and the role of surgery in managing these conditions. Images and videos are presented throughout the module to enhance learning.
This musculoskeletal module focuses on assessing patients with recurrent musculoskeletal conditions and sports injuries, including establishing a management plan with other health professionals. It outlines the differential diagnosis, prevention, management and long-term rehabilitation of plantar fasciitis and chronic ankle instability. In this module, the aetiology, risk factors, presentation, differential diagnosis, examination, imaging and management of Achilles tendinopathy, shin splints, patellar tendinopathy, Osgood-Schlatter’s disease, Carpal Tunnel syndrome, Ilio-tibial band friction syndrome and rotator cuff tendinitis are discussed in detail. The module concludes with the diagnosis and management of elbow epicondylitis and lumbar facet joint syndrome.

Clinical Academic Lead (Back to Base Days) Melbourne Clinical School, The University of Notre Dame
Honorary Principal Fellow Department of Anatomy & Neuroscience, The University of Melbourne
Associate Professor Norman Eizenberg has taught anatomy to medical students (at Melbourne and Monash Universities) and surgical trainees for more than 40 years. His main areas of research and scholarship are in medical education (including student learning of anatomy) and in anatomical variations (including their surgical implications). He was awarded an Honorary Fellowship Degree (in 2016) by the Royal Australasian College of Surgeons in recognition of “significant work in anatomy and of contributions to the College” and is currently Anatomy Specialty Editor for the ANZ Journal of Surgery.
A/Prof Eizenberg’s biggest role was project leader of the recently completed ANATOMEDIA Online which is a comprehensive, interactive learning platform exploring anatomy from multiple perspectives. So far, ANATOMEDIA has received four national or international awards, including the Australian Publishers Association "Best teaching & learning package in tertiary education" (in 2008).
Meanwhile, he managed to keep his hand in clinical practice after-hours as a GP and received Life Membership “for 30 years extraordinary service as a volunteer doctor at matches” by AJAX Amateur Football Club. He was also fortunate to be a Victorian Australian of the Year Finalist (in 2014) for “outstanding contribution: anatomist, doctor and educationalist”.
Outside interests besides organised sport include nature walks and contemporary music. A/Prof Eizenberg is a bit of a film buff and reads books on biography or history (which like anatomy and unlike him, never become outdated).

General practitioner
A native Queenslander, Dr Huddy Fuller graduated from the University of Tasmania in 2012, and spent his hospital years in Launceston then Hervey Bay. He went on to complete GP Fellowship in NSW, choosing general practice because he believes it is the most important medical speciality for the betterment of people’s lives.
Dr Fuller has a background as an exercise physiologist and enjoys bringing this knowledge to general practice. He is experienced in skin cancer screening and management, musculoskeletal medicine, and chronic disease management especially type 2 diabetes. Dr Fuller focuses on an education and shared decision making approach to general practice.
He is heavily involved in the team sport Ultimate Frisbee.

General practitioner
Dr Anoop Jalota is a general practitioner who has special interests in emergency procedures and musculoskeletal medicine. He is passionate about helping patients to quit smoking and manage their weight. Dr Jalota is currently a cluster leader for Central Illawarra and has a passion for continued learning and mentoring.


Senior Lecturer, Exercise Physiology, School of Sport and Health Sciences, Cardiff Metropolitan University, Wales
Dr David Pugh is a Senior Lecturer in Exercise Physiology within the School of Sport and Health Sciences at Cardiff Metropolitan University, Wales. His global research agenda focuses on how regular exercise and physical activity can effectively prevent and treat cardiovascular and metabolic diseases across the lifespan.

Podiatrist & physiotherapist
Ronnie Bateman attained his professional qualifications from LaTrobe University, Melbourne. In 1995, he graduated with a Bachelor of Physiotherapy and returned to study a Bachelor of Podiatry and a Masters of Musculoskeletal Physiotherapy.
Mr Bateman has worked in several sectors including elite sport, aged care and disability, occupational, public health, and private practice.
As a clinician, he promotes treatment pragmatism, and concedes that there are exceptions to most supported clinical and research-based beliefs.
As a podiatrist, he enjoys the challenge of complex foot/ankle conditions, in addition to assisting more proximal pathologies (such as knee pain) by altering distal biomechanics. Podiatric interventions he adopts can include one or more of the following: shoe alterations, insole alterations, over-the-counter orthotics, hand-made insoles/orthotics, strapping, padding, and off-loading. He continues to make devices from casting to fitting where necessary.
As a physiotherapist, Mr Bateman will consider evidence-based research and “old-school” manual therapy options in an attempt to make maximum improvement in the shortest timeframe.
As a lower-limb musculoskeletal practitioner, he can apply top-down (physiotherapy based) and bottom-up (podiatry based) approaches.
Principles and philosophies supported include:
from $1695
.
*provided an outcome measurement activity with a minimum of 5 hours is completed.
Bundle two courses and save 5%, or three courses and save 10% upon enrolment.
Talk to us about deferred payment options, registrar scholarships and special rates.
*For Australian residents only: Online course prices are shown exclusive of GST. If you are GST-registered, please enter a valid ABN at checkout to ensure GST is not applied. Otherwise, 10% GST will be added at checkout. View our FAQ for more information.


HealthCert courses have become the standard by which you gauge all others.
Dr K. Abolarinwa
Good, courses with excellent speakers. I particularly enjoyed the case study scenarios which helped to integrate the knowledge gained.
Dr A. Tucker
This is the pathway to improve your confidence and evolve into the GP you aspire to be.
Dr S. Shinwari
| RACGP Activity Number | ACRRM Activity Number | Activity Title | Education Hours | Performance Hours | Outcome Hours | ||
|---|---|---|---|---|---|---|---|
| 448427 | 38523 | Rheumatoid arthritis | 448427 | 38523 | 4 | 6 | 0 |
| 448705 | 38546 | Degenerative joint diseases | 448705 | 38546 | 4.5 | 6 | 0 |
| 448438 | 38524 | Neck injuries in sport | 448438 | 38524 | 3.5 | 6 | 0 |
| 448711 | 38549 | Low back pain | 448711 | 38549 | 4 | 6 | 0 |
| 448717 | 38551 | Recurrent musculoskeletal and sports injuries in men | 448717 | 38551 | 5 | 6 | 0 |
| 448689 | 38536 | GP Cases- Acute musculoskeletal and sports | 448689 | 38536 | 5 | 6 | 0 |
| 448419 | 38146 | Musculoskeletal Pain | 448419 | 38146 | 4.5 | 6 | 0 |
| 448692 | 38541 | Physical and Biomechanical assessment of lower limb and gait problems | 448692 | 38541 | 7 | 6 | 0 |
| 802660 | 38554 | Low back pain Outcome Improvement Activity | 802660 | 38554 | 0 | 0 | 8.5 |
| Total hours | 37.5 | 48 | 8.5 | ||||
The optional Musculoskeletal Medicine workshop is accredited for 11.5 CPD hours total.
Education hours: 5.5
Performance hours: 6
View the CPD Hours for all HealthCert Education activities.
The purpose of outcome measurement activities is to improve your clinical confidence in managing an identified learning gap. Outcome measurement activities are not a requirement of our Professional Certificate of Advanced Certificate courses; they are a requirement for Australian CPD purposes.
HealthCert Education provides a variety of outcome measurements activities to suit your needs:
The Professional Certificate of Musculoskeletal & Sports Medicine is for degree-qualified medical professionals who wish to learn how to improve patient outcomes, especially those patients with musculoskeletal conditions commonly seen in general practice.
This course is for physicians and degree-qualified medical professionals. There are no prerequisites.
Participants do not need to complete the online course before they are eligible to attend the practical workshop.
Participants do not have to pass an IELTS test but, as the courses are delivered in English, proficiency in listening, reading and writing English is assumed.
Participants will require access to a computer/laptop, an internet connection and a basic level of technology proficiency to access and navigate the online learning portal.
Professionally recognised qualifications and prior studies may be recognised for entry into this course if the learning outcomes match exactly. Please ask a HealthCert Education Advisor for an individual assessment of your prior qualifications and experience.
This certificate course meets the minimum 50 hours CPD annual requirement across all three mandatory CPD activity types, provided an outcome measurement activity with a minimum of five hours is completed. You may use an optional HealthCert outcome measurement activity or develop your own.
Outcome measurement activities are not a requirement of Professional or Advanced Certificates.
Upon successful completion of the course requirements, course participants will receive the Professional Certificate
This certificate course:
To learn more about the delivery of certificates in Australia and overseas, please visit our FAQs.
Professional Diploma Pathway
This course is the first stage of the three-part professional diploma pathway. The full pathway is Professional Certificate of Musculoskeletal & Sports Medicine, Advanced Certificate of Musculoskeletal & Sports Medicine, and Professional Diploma of Musculoskeletal & Sports Medicine.
This organisation is an RACGP-accredited CPD provider under the RACGP CPD Program.




Don't see your question? Explore other faqs or talk to us.
The workshop is fully practical with an expectation that all participants will be fully immersed and practise the teachings on each other. Therefore, there is a strict dress code: all participants must wear T-shirts and shorts to the practical sessions.
Fees will vary based on the program and study option selected (fully online vs online + optional practical workshop). Payments can be made upfront or in monthly instalments. Special rates and various payment options are available. GP registrars and doctors in training enjoy a scholarship of up to $500. Talk to us to learn more.
Completion of any HealthCert course or attendance at an event will enable you to access the HealthCert Alumni Program which includes:
HealthCert Education is pleased to issue digital credentials for alumni. Digital credentials are a permanent online record of your successful completion of a HealthCert course and are issued to all course participants in addition to PDF certificates. If you are based in Australia, you also have the option to order a hard copy of your digital certificate for a small additional fee.
The recommended study duration of this certificate course is 85.5 hours, which includes study of the pre-course activities and readings, online lectures, live tutorials, and online assessment. This self-paced course offers the flexibility of 100% online study in your own time, at your own pace, in your own home or office, with no mandatory face-to-face requirements. You are not required to be online at specific times but can view and replay video lectures at your convenience.
All HealthCert courses meet World Federation of Medical Education standards. This certificate course qualifies for CPD hours from the Royal Australian College of General Practitioners (RACGP) and the Australian College of Rural and Remote Medicine (ACRRM) in Australia. It is recognised by the Royal New Zealand College of General Practitioners (RNZCGP) in New Zealand. It is recognised by the Hong Kong College of Family Physicians (HKCFP) in China. It is a self-submitted activity in Dubai and the United Kingdom. It is a self-submitted activity through the College of Family Physicians in Canada. If you live or work outside one of the above-mentioned countries, please contact us on admin@healthcert.com to discuss whether this course can be recognised in your country.
Course/workshop cancellations and transfers policy
Should you be unable to attend a course or practical workshop you have registered for, please inform us asap at admin@healthcert.com so we can make your place available to waitlisted doctors.
Charges may apply for course/workshop cancellations and/or transfers. Click here for details.
Want to stay up-to-date with the latest case studies, podcasts, free video tutorials and medical research articles pertinent to primary care?
Our Education Advisors can assist you with queries, help you claim special rates and set up deferred payments, and tailor your education pathway to suit your current expertise, interests, and career goals.